11.12.18
Patient studies of a new sensing device have proved it can provide early warning of the potential failure of breast reconstruction surgery, making it easier to take effective remedial action.
Funded by the Engineering and Physical Sciences Research Council (EPSRC) and led by Imperial College London, an international team has developed the wireless “bio-patch” as part of the Smart Sensing for Surgery project.
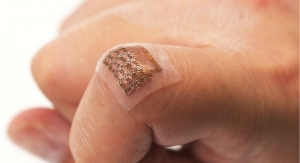
Incorporating electronics measuring just 1.8 x 1.1 cm, the bio-patch was attached to a group of patients for 48 hours following breast reconstruction surgery.
It successfully performed continuous monitoring of the level of oxygen saturation in transferred tissue—a key indicator of whether there is a risk of reconstruction failure.
“Clinical signs of failure often occur late and patients may be returned to the operating room on clinical suspicion,” said Professor Guang-Zhong Yang, director of the Hamlyn Centre at Imperial College London, who has led the Smart Sensing for Surgery project. “Our new bio-patch tackles this problem by providing objective data as an early warning system for medical staff, enabling earlier and simpler interventions, as well as giving patients increased peace of mind.”
Breast reconstruction surgery following a mastectomy routinely includes a transfer of the patient’s own tissue to help rebuild the breast. This procedure achieves high success rates but early detection of possible problems could help further reduce post-surgical complications and cut surgery failure rates.
“This Smart Sensing for Surgery project is an excellent example of how science and engineering can have direct impacts on people’s lives,” said Professor Lynn Gladden, EPSRC’s executive chair. “Spotting post-surgery problems early can help clinicians treat patients quickly and improve outcomes.”
Harnessing a technique known as near-infrared spectroscopy, the new device safely captures and transmits data using sensors hermetically sealed inside fully biocompatible materials. The data is encrypted to ensure security and privacy.
Early trials have opened up the prospect of the bio-patch becoming available for widespread clinical use within 2-3 years. The project team is currently exploring the scope to secure commercial or National Institute for Health Research support for the next stage of development and commercialization.
The device is now being adapted to help monitor conditions such as dementia and chronic obstructive pulmonary disease (COPD).
Smart Sensing for Surgery has achieved other promising advances, including development of sensors that can be implanted just under the skin to provide continuous measurement of pulse rate, temperature and pH balance, for example, and development of “smart” catheters or drains enabling problems (e.g. relating to infection) to be spotted early on.
Funded by the Engineering and Physical Sciences Research Council (EPSRC) and led by Imperial College London, an international team has developed the wireless “bio-patch” as part of the Smart Sensing for Surgery project.
Incorporating electronics measuring just 1.8 x 1.1 cm, the bio-patch was attached to a group of patients for 48 hours following breast reconstruction surgery.
It successfully performed continuous monitoring of the level of oxygen saturation in transferred tissue—a key indicator of whether there is a risk of reconstruction failure.
“Clinical signs of failure often occur late and patients may be returned to the operating room on clinical suspicion,” said Professor Guang-Zhong Yang, director of the Hamlyn Centre at Imperial College London, who has led the Smart Sensing for Surgery project. “Our new bio-patch tackles this problem by providing objective data as an early warning system for medical staff, enabling earlier and simpler interventions, as well as giving patients increased peace of mind.”
Breast reconstruction surgery following a mastectomy routinely includes a transfer of the patient’s own tissue to help rebuild the breast. This procedure achieves high success rates but early detection of possible problems could help further reduce post-surgical complications and cut surgery failure rates.
“This Smart Sensing for Surgery project is an excellent example of how science and engineering can have direct impacts on people’s lives,” said Professor Lynn Gladden, EPSRC’s executive chair. “Spotting post-surgery problems early can help clinicians treat patients quickly and improve outcomes.”
Harnessing a technique known as near-infrared spectroscopy, the new device safely captures and transmits data using sensors hermetically sealed inside fully biocompatible materials. The data is encrypted to ensure security and privacy.
Early trials have opened up the prospect of the bio-patch becoming available for widespread clinical use within 2-3 years. The project team is currently exploring the scope to secure commercial or National Institute for Health Research support for the next stage of development and commercialization.
The device is now being adapted to help monitor conditions such as dementia and chronic obstructive pulmonary disease (COPD).
Smart Sensing for Surgery has achieved other promising advances, including development of sensors that can be implanted just under the skin to provide continuous measurement of pulse rate, temperature and pH balance, for example, and development of “smart” catheters or drains enabling problems (e.g. relating to infection) to be spotted early on.